Have you enrolled in Medicare? If so, you may have questions regarding coverage requirements and out-of-pocket costs related to sleep apnea diagnosis and treatment. Dr. Victoria Uryniak and Dr. Carson Ferris-Zeolla help patients experiencing sleep apnea symptoms obtain the treatment they deserve. At the same time, our office assists patients in understanding what to expect from their Medicare plan. Call us at (908) 200-7007 to set up a visit to talk about Medicare and your sleep apnea signs at our practice located in Clinton, NJ.
What Is Sleep Apnea?
Sleep apnea happens when a patient’s airways become blocked during sleep. This blockage stops the flow of air in and out of the body, often resulting in a sudden snore, snort, or gasp. In severe cases, about 30 of these sleep apnea events can occur every hour.
Without treatment, sleep apnea deprives people of needed rest and oxygen. Over time, undiagnosed and untreated sleep apnea can lead to serious problems including memory loss and an increased risk of cardiovascular disease.
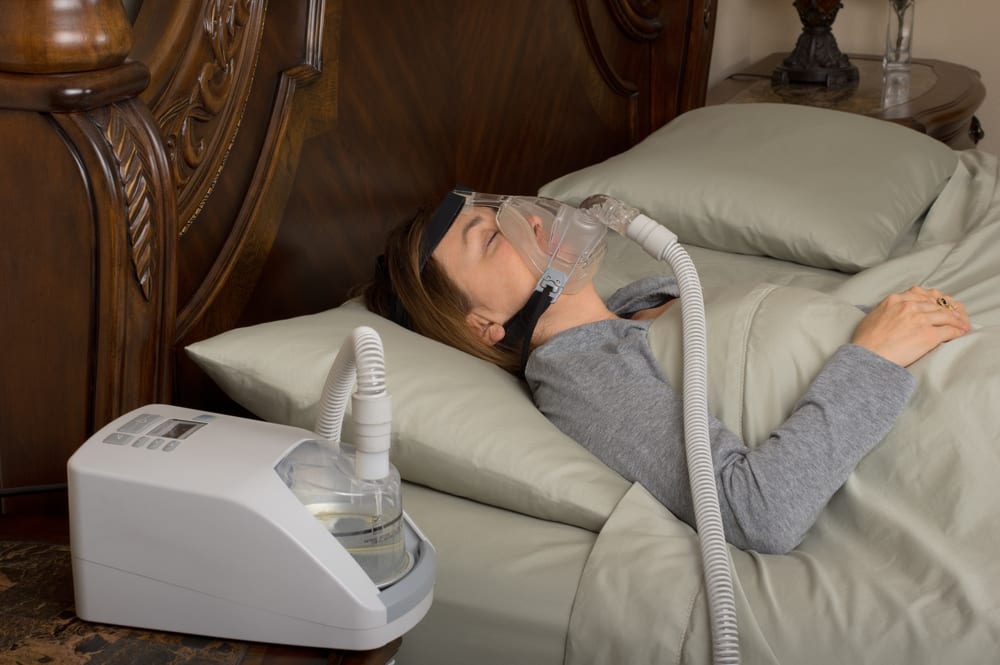
Dentists regularly help diagnose and treat individuals with sleep apnea. Common treatment methods include customized oral appliances and occlusal adjustments. In some situations, a patient may also find a CPAP machine helpful to keep the soft palate and other tissues from collapsing into the throat during sleep.
Who Pays for Sleep Apnea Diagnosis and Treatment?
Many private insurance companies cover some or all of the cost of sleep apnea diagnosis and treatment. However, Medicare is a government-run program with its own set of coverage requirements. Anyone who is currently covered by Medicare or expects to be in the future should understand guidelines related to sleep apnea diagnosis treatment.
Information on Medicare for Sleep Apnea Patients
Want a better understanding of Medicare sleep apnea related coverage: read through these helpful information bullet points:
- Medicare Part B covers medical and outpatient sleep disorder services. If you are admitted to the hospital as a result of sleep apnea, you would receive coverage under Medicare Part A. However, Medicare Part B is necessary for coverage of some or all of your obstructive sleep apnea diagnosis and treatment. Not sure if you are covered under Medicare Part A, Part B, or both? Contact Medicare.
- At-home sleep tests for sleep apnea may be covered under Medicare Part B. Typically, Medicare Part B covers sleep laboratory conducted tests. The program may also cover some or all of the cost for an at-home sleep test ordered by your dentist in Clinton, NJ.
- Continuous positive airway pressure (CPAP) machines may be covered by Medicare Part B for at least three months. In addition to any treatments you receive from your dentist, such as creation of an oral appliance, the cost of a CPAP machine rental may be covered by Medicare for three months. After the three-month period, Medicare may extend coverage if CPAP therapy produces positive outcomes.
- Oral appliances may be covered under Medicare Part B. If your at-home sleep test or sleep lab test indicates an obstructive sleep apnea diagnosis, you may try an oral appliance to lower your nightly sleep apnea events. Sometimes, costs related to the construction of oral appliances is covered by Medicare B, especially if the oral appliance is prescribed within the initial three months of sleep apnea treatment.
Talk to Your Dentist About Medicare and Sleep Apnea Treatment
Still unsure about your financial commitments and responsibilities regarding sleep apnea diagnosis and treatment? Our team of finance experts at Walnut Pond is happy to discuss your options. You can pay for some services through the third-party CareCreditⓇ financing program or via your Medigap plan.
Contact us today for more information or to schedule a sleep apnea evaluation.